Laser Surgery
Laser surgery corrects vision (short/long sight, astigmatism) by reshaping the cornea. For more information on the various options, jump to the relevant section below:
Yag Laser Capsulotomy
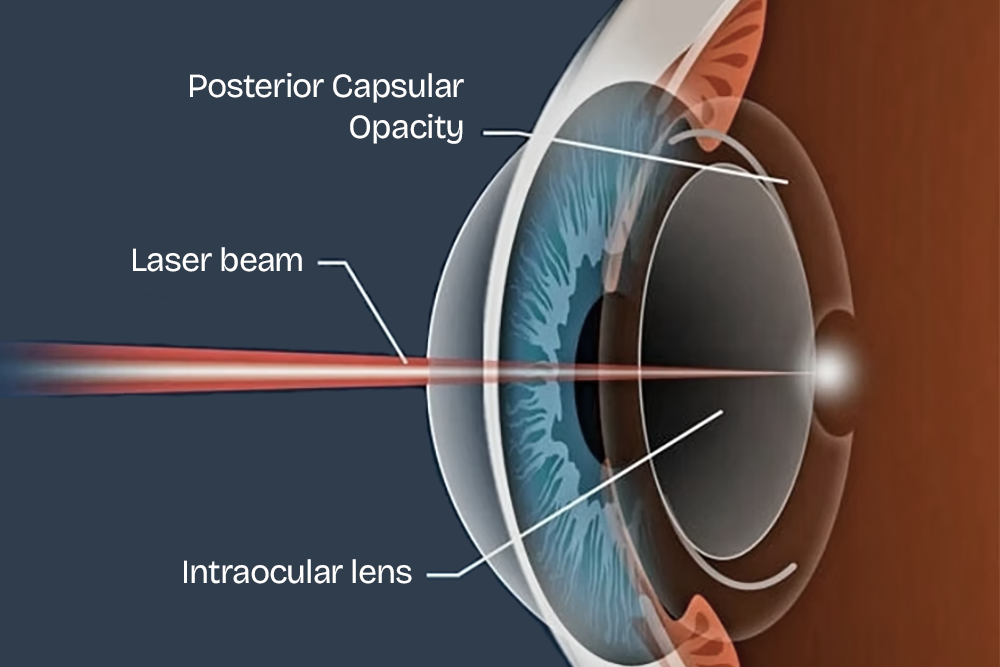
YAG (yttrium-aluminum-garnet) laser capsulotomy is a non-invasive outpatient procedure used to treat posterior capsule opacification, a common condition after cataract surgery where the lens capsule becomes cloudy, causing blurred vision.
Effectiveness: Highly effective, with most patients experiencing significant vision improvement. The procedure is typically needed only once.
Procedure:
- Preparation: Eye drops are given to dilate the pupil and numb the eye. They sting a little on instillation.
- Procedure: The procedure is performed in the clinic. A sterile contact lens is placed on the eye, helping keep it open and providing a clear view for the laser treatment. A focused YAG laser creates a small opening in the cloudy posterior capsule, allowing light to pass through clearly. The procedure takes a few minutes per eye.
- Duration: The procedure takes around 5–10 minutes.
- Recovery: Painless, with minimal discomfort. Vision typically improves within hours, and patients can resume normal activities soon after.
Risks:
- Floaters are common after the treatment, but these will gradually become less noticeable.
- Other problems are extremely rare. There have been reports of issues that can result in recued vision, but these are rarely seen in practice
- Risk of fainting during or after the procedure (vasovagal syncope)
Laser Peripheral Iridotomy
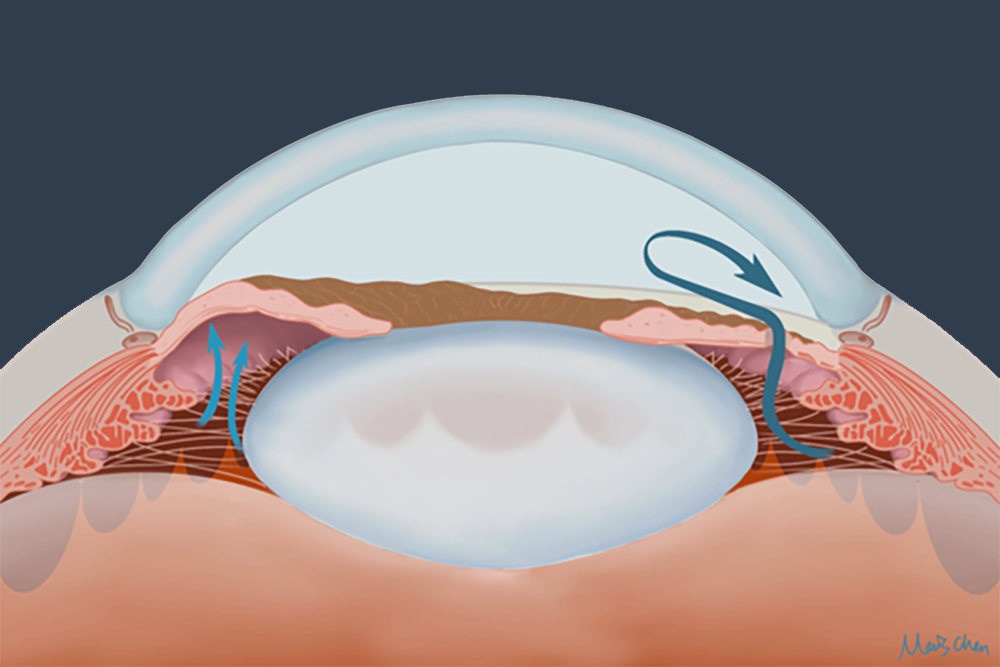
Laser Peripheral Iridotomy (LPI) is quick and gentle procedure used to treat or prevent angle-closure glaucoma, a condition where blocked drainage pathways in the eye cause increased intraocular pressure (IOP), potentially damaging the optic nerve. LPI creates a small hole in the iris to improve aqueous humour flow, relieving pressure buildup.
Benefits
- Prevents Acute Angle-Closure Attacks: LPI can be effective in preventing sudden, painful glaucoma attacks in patients with narrow or closed angles.
- Prophylactic Use: Reduces chance of developing angle-closure glaucoma in patients at risk, by 50%.
- Long-Lasting: A single LPI typically provides lifelong protection against angle-closure in treated eyes.
Procedure
- Pre-procedure: Drops to constrict the pupil are given before the procedure. These often give an achy feeling around the eyes for a few hours. You will also be given IOP lowering drops before and after.
- Anaesthesia: Topical anaesthetic eye drops
- Laser Application: The procedure is performed in the clinic. A contact lens is used to keep the eye open and improve the view for the treatment. A focused laser beam creates a tiny opening in the peripheral iris, allowing fluid to flow between the anterior and posterior chambers of the eye. Usually, 5-10 shots are needed per eye. The laser causes a moment of sharpness when fired, but it is very well tolerated.
- Duration: The procedure takes around 5–10 minutes.
- Recovery: You will be given anti-inflammatory drops for 1 week, which should help settle any symptoms. You may have slightly blurry vision, or sensitivity to light, that should settle within a day or two. Most patients resume normal activities within a day.
Risks
- Mild Side Effects: Temporary blurred vision, mild inflammation, or light sensitivity.
- Rare Complications: IOP spikes, bleeding, or lens damage are uncommon but possible. Light can sometimes enter through the opening, and lead to a visual disturbance. Usually this gets less noticeable with time.
- Risk of fainting during or after the procedure (vasovagal syncope)
- Variable Efficacy: In some cases, additional treatments may be needed if the angle remains narrow or IOP is not adequately controlled.
Further information:
https://glaucoma.uk/about-glaucoma/treatments-surgery/laser/
Selective Laser Trabeculoplasty (SLT)
Selective Laser Trabeculoplasty (SLT) is a very gentle and successful laser treatment to reduce the intraocular pressure (IOP) in patients with open-angle glaucoma or ocular hypertension. SLT uses laser to cause gentle inflammation in the eye’s trabecular meshwork, a tissue in the eye responsible for draining aqueous humour, to improve fluid outflow and reduce IOP.
It is effective in around 80% of patients, with a reduction in eye pressure by around 20-30%. The risk of side effects with the laser is extremely low. The effect of the laser does wear off with time, lasting on average 3 years, but it can be repeated numerous times.
SLT has been performed for more than 30 years, but over the last decade it has been used much more frequently as a first line treatment. This has a huge advantage, as it can prevent the need for daily eye drops and the associated potential side effects.
Procedure
- Pre-procedure: Drops to constrict the pupil are given before the procedure. These often give an achy feeling around the eyes for a few hours. You will also be given IOP lowering drops before and after.
- Anaesthesia: Topical anaesthetic eye drops are used to ensure patient comfort. They sting a little on instillation
- Procedure: This treatment is performing in the clinic. A contact lens is used to keep the eye open and to view the tissue requiring treatment. 100 shots of low-energy laser is applied around the circumference of the eye. The laser is very gentle, but the eye will feel a little achy as the treatment progresses.
- Duration: The procedure typically takes 5–10 minutes.

Effectiveness:
- Effective IOP Reduction: SLT lowers IOP by 20–30% in 80% of patients, comparable to topical glaucoma medications.
- Long lasting: The effect of the laser lasts 3 years on average.
- Repeatable: Unlike older laser treatments, SLT can be safely repeated when the effect diminishes over time.
- Minimal Side Effects: SLT has a low risk of complications, with mild, transient side effects for the vast majority of patients.
- Medication Reduction: Successful SLT may reduce or eliminate the need for glaucoma medications in some patients.
Risks:
- Most patients will have a bruised feeling in the eyes, with some light sensitivity for a day or two after the procedure. Paracetamol and/or Ibuprofen (if no contraindication) can be helpful to alleviate symptoms. The vision is usually unaffected.
- 1 in 200 risk of significant inflammation, usually treated with a drop course.
- 1 in 50-100 risk of temporary IOP spike, typically treated with drops and/or tablets.
- Risk of fainting during or after the procedure (vasovagal syncope)
Further information:
https://glaucoma.uk/about-glaucoma/treatments-surgery/laser/
Discussion with Duncan is important to answer any questions that you may have. For information about any additional conditions not featured within the site, please contact us for more information.








